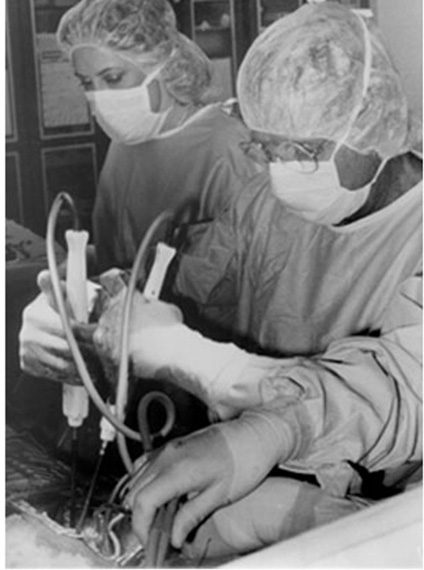
Photo courtesy INTEGRIS.
[dropcap]Zuhdi’s[/dropcap] dream was to build a successful heart-lung machine to pump sufficient oxygen to keep the organs alive during an open-heart procedure.
While Zuhdi was ostensibly training in Dennis’s laboratories, the experienced cardiologist and scientist recognized a momentous mind when he saw it. He later wrote of Zuhdi:
[pullquote]All of a sudden, at 27 years old, I became the most known worker in heart-lung machines in the world.[/pullquote]“During his training at Brooklyn, Zuhdi was a very bright star among the 50-odd residents in training there, always ready with suggestions and the drive to carry them through, which he did regularly in the year he worked with me in the research laboratory during our work on developing a pump-oxygenator, as a result of which, we were able to salvage the first long-term survivor of massive myocardial infarction and shock by temporary circulatory support with that same pump-oxygenator.”
Dennis’s matter-of-fact tone belies the revolutionary medical milestone he and Zuhdi had achieved. On Nov. 1, 1954, the duo made history with their new assisted circulation machine.
“We used it on a patient who was in total heart failure,” Zuhdi recalls. “We used it for the first time in the world to help that patient who was in a coma. And basically it worked. It was the first successful case in the world of a heart-lung machine being used as an assisted circulation to a failing heart. … All of a sudden, at 27 years old, I became the most known worker in heart-lung machines in the world. They used to come visit Dennis in the lab, and he would always wave them over to me. ‘Tell them how you did it!’ And that was Dennis, you know.”
‘You Need Oklahoma’
Zuhdi’s assisted circulation machine had been a success and brought him instant worldwide fame, but his mind was not content to rest.
“With Dennis, we were basically working on how to duplicate the human body.” He chuckles and rolls his eyes, amused. “To duplicate God’s creation!”
Meanwhile, at the University of Minnesota, a surgeon-scientist name C. Walter Lillehei – so-called The King of Hearts – was taking assisted circulation one step farther by using cross-circulation, or a compatible human being as a heart-lung machine. At Dennis’s urging, Zuhdi joined Lillehai in Minnesota in 1956.
“He was very smart,” Zuhdi says, wagging his finger. “At the time, many thought it was very stupid. To them he was a kook. But he was smart.”
As Zuhdi worked with Lillehai to perfect assisted circulation, word of Zuhdi’s accomplishments were reaching the ears of an enterprising Oklahoma surgeon: Dr. John Schilling, the new chairman of the University of Oklahoma Department of Surgery. Schilling was determined to establish a preeminent heart surgery research section at the OU College of Medicine, and he wanted Zuhdi there to build it.
Oklahoma seemed an unlikely home for one of the world’s foremost cardiac scientists. As Zuhdi says, “It had nothing of science at the time.”
But Dennis and Lillehei encouraged the move, telling Zuhdi he could become “The King of the Prairies.” Dennis told him, “Go. You don’t need me anymore. You need Oklahoma.”
Zuhdi never looked back and never left the state he has called home for most of his life. In 1957, he joined the OU College of Medicine in Oklahoma City. He was delighted at Schilling’s willingness to build him a lab. In that lab, Zuhdi built his latest version of the heart-lung machine. Schilling could not have been more thrilled with his recruit.
“He was so elated,” Zuhdi remembers. “He was like a child. Nobody had heart-lung machines except two or three universities. And they were lousy.”
But Zuhdi’s stay in the OU Department of Surgery was too brief for Schilling and the university’s administrators. He was told by the department that as a member of a state university, his work was to be overseen by a committee of three members, and that was a dealbreaker.
“I never ask others what I want to do,” Zuhdi says emphatically. “This my life. This is true. My rules.”
Beacon Of Hope
For Zuhdi, the choice was a no-brainer. He would not tolerate committee oversight of his research. Although he credits Shilling with bringing him to Oklahoma, and the two remained lifelong friends, Zuhdi severed all ties to OU. Luckily, while Oklahoma was an unrealized state for scientific and medical innovation, visionaries abounded in Oklahoma City at the time. One such luminary was John Kirkpatrick. When Kirkpatrick discovered that Zuhdi intended to leave the state, he offered to build the scientist a lab anywhere he wanted – as long as he stayed in Oklahoma.
“So we rode around in his car, and I chose the worst-looking hospital in Oklahoma City,” Zuhdi says with a laugh. “Mercy on 13th Street. I said ‘Here.’ Because really, a hospital, I don’t need. I just needed a lab.”
And thus was born the Mercy Hospital Heart and Research Institute-Experimental Laboratory.
It was in this new lab that Zuhdi turned his mind again to perfecting the heart-lung machine and the survival for patients of cardiac surgery. The problem, he determined, was the blood itself. The amount needed to replace lost blood during open-heart surgery, and to keep circulation flowing to the oxygen-starved heart and lungs, was staggering. In addition, blood could barely flow through constricted arteries. Open-heart surgery was still a deadly business for many patients, despite the astronomical advances that had been made in the previous several years. Zuhdi now had a new goal to tackle.
What, he wondered, would happen if sugar water were used?
Zuhdi holds up his hand, his forefinger curled into a tiny circle against his thumb.
“This is why they died,” he says, indicating the small opening in his fist to mimic the constricted artery. “Then, we add the sugar water, and PEW!”
He widens the circle of his finger and thumb as far as it can go.
“It blew up! PEW! The way the brain comes upon it …” he shakes his head in wonder.
The priming of the heart-lung machine with a calculated volume of non-hemic primer is now known as total intentional hemodilution, and Zuhdi’s technique is used to perform cardiac surgery and transplants on millions of patients each year. The first, however, was a child from Broken Bow named Terry Gene Nix. At a year old, Terry Gene had been diagnosed with pulmonary valvular stenosis, in which the valve that controlled blood flow to his tiny heart and lungs was narrowed, taxing his under-oxygenated organs. As he grew older and his condition deteriorated, little Terry Gene didn’t have much time. He was 7 years old in 1960 and about to become the first human recipient of total intentional hemodilution in the world.
To the delight of his family, doctors and the medical community around the world, Terry Gene only needed a fraction of the replacement blood needed to keep oxygen circulating during his surgery – some 1.5 pints, as opposed to gallons. The day after his three-hour procedure, he was smiling for the cameras of the world.
Although Terry Gene died three years later from an unrelated ailment, he served as a beacon of hope for patients and surgeons across the globe. Because of him, millions of patients each year undergo open-heart surgery and transplants using total intentional hemodilution. Terry Gene’s grave marker reads:
Terry Gene Nix
The Gateway to All
Total Intentional Hemodilution
By Whom Millions Have Come To Life
February 25, 1960
Remembrance by Nazih Zuhdi, M.D.























